
Jack's Journey
Story 120
Chelsea Holder was lying in a hospital bed, her heart and mind racing as nurses surrounded her.
She wasn’t supposed to be here. She was only 29 weeks pregnant. Just hours earlier, she was in a routine check-up with her OB/GYN, who only sent her to the hospital as a precaution when she saw her blood pressure was abnormally high — about 180/110.
Now, nurses were racing in and out of Chelsea’s room, routinely checking her blood pressure and praying it would go down. Hoping they wouldn’t have to rush into an emergency cesarean section, Chelsea couldn’t bear to look at the number on the monitor.
“Is it bad?” she asked, looking to her husband, Harris. “Is it bad?”

Chelsea was hooked up to an IV to help her relax. Nurses waited another 45 minutes before checking again as Chelsea tried to calm down, but just the sight of the blood pressure cuff gave her anxiety.
They read her vitals again. High.
Chelsea looked to Harris, defeated. Until that moment, she maintained hope that they would be going home. Instead, nurses at Adventist Health Glendale began preparing an operating room. For the health of herself and her baby, she would have to deliver that night. She was awash in fear.
“I remember basically thinking, ‘I could die. He could die. We both could die,’” Chelsea said.
Her doctor’s last words to her before sending her to the hospital reverberated in the back of her mind: “You don’t want to have a baby at 29 weeks.”
It was Chelsea’s first pregnancy, and she didn’t know what to expect. She would have never expected this.
“I remember basically thinking, ‘I could die. He could die. We both could die.’”
In the operating room, Chelsea squeezed Harris’ hand during a 45-minute-long surgery that felt like an eternity. Her mind continued to race with questions: How long will this procedure take? Will my baby be OK? Will I be OK?
And then, a soft cry interrupted her thoughts. Chelsea was lost in a wave of relief.
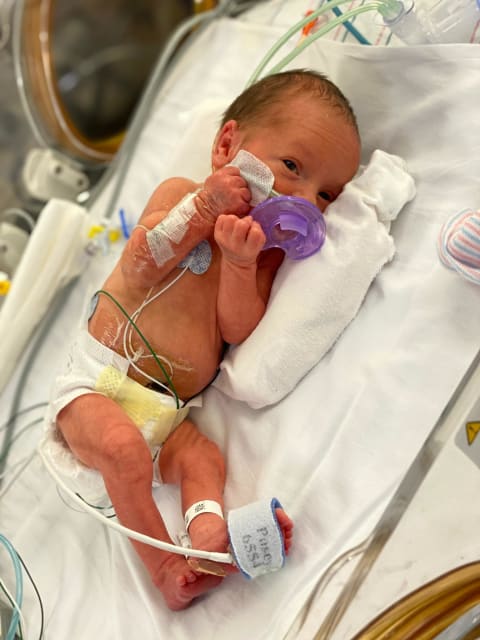
Jack Sherman was born January 13, 2021, weighing 3 pounds 7 ounces and arriving 11 weeks earlier than planned.
“Thank God. Thank everything in the entire universe,” Chelsea recalled thinking. “Even though we had a huge journey ahead of us, I just thought: ‘He’s alive, and now we’re going to do whatever we need to do to get him to survive.’”
Because he was born premature, Jack spent the next six weeks at Adventist Health Glendale’s Level III-B Neonatal Intensive Care Unit, where he received specialty care. Chelsea found it comforting to have professionals around Jack 24 hours a day to ensure his well-being and also viewed the NICU stay as a learning experience for her. While there, nurses taught her how to feed, how to change a diaper and how to care for her baby.
Because of COVID-19 restrictions, only one parent was allowed in the NICU at a time. Chelsea and Harris would trade off visiting him. Chelsea would go for two hours each morning and Harris would visit for two hours in the evenings.
“We developed a little kinship and family in the NICU,” Chelsea said.
It’s a testament not only to the vulnerability of the situation, but also the sensitivity of the associates working in the NICU, Chelsea shared. Nurses, doctors, developmental therapists, and others on the unit saw Chelsea at her most vulnerable, her most frightened, and her most uncertain about what would come next.

Chelsea felt an instant connection to one person in particular — a nurse named Chris Emmons. Her warm Scottish accent reminded Chelsea of the years she spent living in England while in college. Her straightforward advice and lessons for the first-time parents were “priceless,” Chelsea said.
“I really looked up to her,” Chelsea said. “I cried when we left because we weren’t going to have that safety net and friendship with those people we were with every day.”
By the time that Jack was ready to go home, he had gained about four pounds and was 36 weeks old. As Chelsea and Harris walked out of the hospital, picked Jack up, and secured him in his car seat, a peaceful quiet washed over them.
It was the first moment, they realized, that Jack was away from the hustle and bustle of a hospital — the first time he wasn’t hearing the ever-present hum of machinery and chirps of heart rate monitors.
It was the first moment that Chelsea realized that finally, after six weeks, they were together as a family.

Jack is 18 months old now, healthy and thriving.
He still receives check-ups with an Adventist Health developmental therapist to ensure he is on track to reach all of his milestones — a seamless transition of care that Chelsea said brings her comfort.

On his first birthday, Jack didn’t just eat cake and look cute. He and his family raised more than $2,500 for Adventist Health Glendale’s NICU as a way to express gratitude for the care they received.
Meanwhile, Chelsea — who had pregnancy-induced hypertension with severe features — has been keeping an eye on her blood pressure. She now advocates for women to be aware of their numbers, especially if they are pregnant.
She describes Jack these days as “a big, chunky guy,” who continues gets taller every day. He’s walking now and loves pointing and taking command of any room he enters, Chelsea said.
“We call him the little director,” she said, laughing. “You’d never know that he had such a difficult start. He’s a total warrior.”
Related stories

Todd Reese

Chris Garcia

Randi White

Jeff Musser

Sarah Gutierrez

Cory Ferrier

Juan De La Cruz

Mara Bryant

Diana Erdmann

In His Footsteps

Gary Obreque

Heartbeat in a Bottle

Wes Rippey

Adam Lee

Erasmo Cortez

Heather Thompson

John Hay

Cheri McCall

Valerie's Journey
